
Get Help Kicking the Habit
It’s estimated that 70% of smokers want to quit, and about half of them try each year — often around New Year's resolutions. But only 6% are successful. Quitting smoking is hard. The American Cancer Society recommends that those who want to improve their chances of success take advantage of various support systems, such as:
Online and In-Person Quitting Groups
Smoking Secession Phone Lines
Counseling
Support from Family and Friends
Guide Books
Prescription Medications to Reduce Cravings
Nicotine Replacement Products
“By quitting – even for 1 day,” contends the American Cancer Society, “smokers will be taking an important step toward a healthier life and reducing their cancer risk.” Of course, kicking the habit for good is best, but some amazing things happen when you stop smoking, even if you’re only able to do so for a short period of time.
1) Within 20 Minutes, Your Heart Rate Drops
Nicotine is stimulant that increases heart rates by about 10-20 beats per minute. Considering the average person’s heart beats about once per second, that’s a sizable increase. Tachycardia (the medical term for having a fast heart rate, is classified as having a rate above 100 beats per minute) essentially reduces the effectiveness of the heart because it’s unable to fill fully before it pumps the blood back out. According to the American Heart Association, severe cases may lead to cardiac arrest and unconsciousness, but even mild-to-moderate tachycardia is associated with fainting, lightheadedness, fatigue, and shortness of breath. Although nicotine can stay in the body for up to three days after your body absorbs it, the impact is lessened drastically over time. The CDC reports your heart rate will begin to decline just 20 minutes after having a cigarette.
2) Within 2 Hours, Your Circulation Improves
In as few as two hours, your heart rate and blood pressure may totally normalize. This means that your heart will be more effective at pumping blood throughout your body. If you’re normally the kind of person who feels cold in your hands or feet, the increased circulation will make you feel warmer.
3) Within 12 Hours, Your Carbon Monoxide Levels Normalize
Every aspect of your body relies on oxygen, and your red blood cells normally do a good job of carrying it throughout the body. However, smoking brings carbon monoxide into the body, and this binds to the red blood cells and forms carboxyhemoglobin (COHb), preventing oxygen from being transported. Someone who smokes a pack a day may have 3% to 6% COHb level, while two packs bumps it up to between 6% and 10%. A person who smokes three packs can have a COHb level of up to 20%. Although rare, it has the potential to result in carbon monoxide poisoning—the same thing that happens to people who die in fires. Even lesser COHb saturation levels can result in noticeable symptoms, such as increased heart rate, decreased capacity for exercise, headaches, visual distortions, nausea, confusion, weakness, sleepiness, and flu-like symptoms. The good news is, within 12 hours of your last cigarette, your carbon monoxide levels will normalize according to the CDC.
4) Within 24 Hours, Your Heart Attack Risk Declines
Smoking may increase your risk of having a heart attack by as much as 70%, and it does take a significant amount of time before your risk declines to normal levels. However, just 24 hours after you put out your last cigarette, your risk starts to drop. After about a year, your risk is cut in half, and you may be at an average risk level after eight.
5) Within 48 Hours, Your Sense of Smell and Taste Begin to Return
Your ability to taste and smell things are closely interlinked, and smoking inhibits both. On the one hand, vascularization causes the taste buds to become flatter or lose their shape, which impacts their ability to perceive flavors. On the other hand, inhaling toxic fumes from cigarettes damages the nerves and reduces the ability to smell. With scent reduced, the ability to taste different things and appreciate the intensity of flavors diminishes as well. “After 48 hours, your ability to taste and smell improves,” according to Everyday Health. “After 72 hours, it's easier to breathe,” too.
Your Health Improves Over Time
While this page focuses on what happens when you quit smoking right away, the benefits increase over time. According to the CDC, the following milestones apply:
2 Weeks to 3 Months- Heart attack risk decreases further, and lung function improves.
1 to 9 Months- Coughing and incidents of shortness of breath decrease.
1 Year- Heart attack risk is cut in half.
5 Years- Stroke risk reduces. Between 5-15 years after quitting, your risk is cut in half.
10 Years- Risk of dying of lung cancer is cut in half. Risk of other cancers, such as mouth, throat, esophagus, kidney, bladder, and pancreases, also decrease.
RefillWise Can Help
The RefillWise prescription discount card works on medications like Chantix and Zyban, which are often prescribed by physicians to help people quit smoking. It also works on nicotine replacement medications, such as Nicotrol. If you don’t have insurance or your insurance doesn’t cover smoking cessation medications, talk with your physician about which medications are right for you. Then, sign up for your free RefillWise card to reduce your prescription costs and earn cash back to reward yourself for your success.

The holidays are typically joyous, full of celebrations and time with loved ones. Unfortunately, it’s also one of the deadliest times of year due to impaired driving. That’s why each December, the president of the United States issues a memo urging people to partake in National Impaired Driving Prevention Month. Understandably, the focus of most outreach efforts involves creating awareness for drunk driving, but alcohol isn’t the only thing that can impair driving; some medications can as well.
Which Medications Pose Risk?
A number of prescription and over-the-counter medications can impair driving. Moreover, sometimes even small doses of the medications can impair driving if a person has gone off schedule, is mixing medications, or consumes alcohol alongside them. Busy holiday schedules, which also cause some to miss out on sleep, can further enhance the effects of some medications. Research presented by Find Law concludes that the following six categories pose the greatest risk:
Pain Medications: Opiates, including morphine, codeine, and hydrocodone, pose a risk because they naturally make people sleepy, dizzy, or disoriented. However, even pain relievers like ibuprofen and Tylenol that don’t have the same side effects can cause trouble too, as pain tends to exhaust people. Once the pain is diminished, it’s easier to fall into a relaxed state and become drowsy or less aware.
Antidepressants: Some antidepressants work by relaxing an individual. As sedatives, they also impair driving and can cause symptoms that mimic excessive alcohol consumption.
Valium: Often prescribed to relieve anxiety or to reduce seizures, valium is a strong sedative. “10 mg of the popular tranquilizer can cause impairment similar to having a blood-alcohol concentration of 0.10 percent,” according to Find Law.
Antihistamines: Some antihistamines, such as Benadryl, are known to cause drowsiness.
Decongestants: Medications like ephedrine (found in traditional Sudafed) can make people jittery, anxious, and disoriented, while others cause drowsiness.
Sleeping Pills: While most wouldn’t dream of taking sleeping pills and then getting behind the wheel right away, it can take them a considerable amount of time to wear off too. That means some may still suffer from grogginess the morning after taking a sleep aid.
What to Do When Medications Impair Your Driving
Naturally, driving while drowsy, disoriented, or distracted is dangerous, so the primary concern of taking these and similar medications is the risk of causing an accident. However, because of the high number of drunk drivers on the road this time of year, there is also much more patrolling by law enforcement. Those exhibiting any signs of impaired driving have a high likelihood of being stopped. Even those with no alcohol in their systems can still receive a ticket for driving under the influence (DUI) if medications are found in their systems, which comes with the same consequences as a drunk driving charge. To avoid these risks, consider some of the following strategies:
Talk to your doctor. If you’re on a medication that you know impairs your driving, have a frank conversation with your physician about how it impacts your life and see what alternate options are available. Under your doctor’s guidance, you may be able to discontinue, reduce, or change your medication. Other times, talking the medication at a different time of day when you won’t be behind the wheel may be a possibility.
Take public transit. If changing up your medication in some way is not a possibility, see if your region's transit system is. Many major metropolitan areas offer special transportation services for the elderly and disabled which puts it within reach for people who might otherwise have trouble getting to a bus, train, or subway.
Carpool. Just as people who partake in alcohol while out should arrange for a designated driver, those on specific medications can too.
Hail a ride. Taxis or companies like Lyft can often have a driver at your door within minutes, depending on where you live.
RefillWise Can Help
Whether you have medications you need to take regardless, or your doctor recommends you switch to a new medication that isn’t covered by your insurance, RefillWise can help keep your costs lower. Moreover, by using our free prescription discount card, you’ll accrue rewards that you can use on anything from groceries to thank-you gifts for those who are able to fill the designated driver role. Get your RefillWise card by signing up on our site or texting JOIN to 22822.
When authorities found Tiger Woods last May, his vehicle was stopped in the middle of the road and he was slumped over at the wheel. His car was damaged, his tires were flat, and Woods could not perform any of the traditional field sobriety tests. He was later charged with driving under the influence, but it wasn’t alcohol in his system causing the distress. Woods was on a powerful cocktail of meds prescribed to him by his physician to help him manage postoperative pain and sleep.
With several back surgeries now under his belt, as well as a long-running history for making headlines due to his medication habits, Woods has become a bit of a poster child for the ongoing battle America faces with prescription medications. He’s a talented athlete, a public figure, and a father. Now, Woods admits he’s also a man with a problem, and he needs help managing his medications. He’s not alone. More than 20,000 people lose their lives each year to overdoses on prescription pain medications, and those numbers don’t include people who have lost their lives in accidents involving prescription meds either. December is National Impaired Driving Month, and few drivers willfully set out to cause harm. But in the grip of pain, it may be difficult to realize when you have a problem. Please consider the following.

Recognize When You Need Help
Taking pain medication is absolutely necessary for many people. Moreover, taking it after a surgery can help ensure that a person’s body heals well and that they are able to resume normal activities faster. However, it took falling asleep at the wheel and being arrested for Woods to finally acknowledge his situation, and while he should be applauded for having the bravery to seek help, perhaps his arrest could have been avoided if he had noticed signs and taken preemptive action.
Signs to Watch For
According to WebMD, some signs to watch for include:
strong desire to use opioids
inability to control or reduce use
trouble meeting social or work obligations
having legal problems due to drug use
spending large amounts of time to obtain opiates
development of tolerance (meaning the need to use larger amounts over time)
having withdrawal symptoms after stopping or reducing use (such as depressed mood, stomach upset, insomnia, and muscle aches)
How to Talk to Your Doctor
If you recognize any of the signs above or have concerns about the medications you’re taking, it’s important to have a discussion with your doctor. Based on news reports, it seems Woods opted for in-patient treatment, which often includes changing medications and learning more about how specific prescriptions interact and impact the body. However, with your physician’s help, you can make similar changes and lower your risk from home.
1) Remember Your Doctor is Familiar with Your Condition
Many people shy away from these discussions because they fear judgment or believe they’re at fault, but your physician knows the medications he prescribes and understands how they impact people. He will be your biggest ally in managing your prescriptions better, but he needs information only you can provide to do it.
2) Share All Information
Your physician needs to know everything you’re taking, whether it’s simply the prescriptions he has given you, over-the-counter medications like antihistamines, supplements, or things you’ve obtained through other sources. Speak freely about how much of each medication you’re taking, when you’re taking it, what symptoms you have, and how you feel while you have the med in your system. Each bit of information will help him piece together how to best help you.
3) Ask Questions
Each person’s body will respond differently to medications, so it’s important to ask questions if anything seems unclear or doesn’t feel like the right choice for you. Your physician may suggest that you come off a medication entirely or may simply suggest you reduce the amount. Either of these can result in withdrawal, so it’s also helpful to ask about possible withdrawal symptoms, the length of time you’ll need to transition, and details of any new medications he recommends as replacements or to help you manage withdrawal symptoms.
Get Help Early
Woods is one of many public figures who have had issues with prescription pain medications in recent years. Both Prince and Michael Jackson are among those who did not get the help they needed and did not have positive outcomes. This only highlights the importance of paying attention to how your body responds to medications and getting in to see your physician as soon as possible when you think you might need help.
Get Help Managing Your Prescription Costs
If your physician recommends that you switch to a medication that is not covered by your insurance, or suggests you take prescription medication to manage withdrawal symptoms, RefillWise can help. Our prescription discount program works across a broad spectrum of medications and saves people an average of 40%. To get your free RefillWise card, text JOIN to 22822 or sign up on our site today.
We are all caregivers in some way. Perhaps we look after family, friends, neighbors, or even pets, offering medicine or bringing chicken noodle soup when someone is sick, or simply being a compassionate ear when a loved one needs to talk. However, some of us have ventured into extraordinary caregiver journeys. We care for grandparents, parents, spouses, children, and other family members who can no longer care for themselves—those who suffer from Alzheimer’s, dementia, strokes, and other disabilities.
It’s estimated that there are 44 million family caregivers in the United States, providing roughly 75% of all necessary care services. Family members spend about 37 billion hours each year providing care which, if paid, would amount to at least $470 billion in wages annually. What’s more, AARP notes that caregivers spend about 20% of their own wages to provide for those they care for, which amounts to $6,954 on average, or as much as $9,022 per year in certain demographic groups.
If you’re a family caregiver, you probably don’t need to be reminded of your ongoing sacrifices; you know them well. However, in honor of National Family Caregiver Month, we’d like to recognize the work that you’re doing, and provide you with information about a few resources that may be able to ease some of your strain.

1) Support Groups
Although each caregiving journey is unique, many of the challenges individual caregivers face share similarities — from trying to carve out “me” time, to navigating the medical community, sorting through government benefits and insurance plans, and more. On top of this, caregiving can be emotionally trying as well. It helps to have support from others who are working through similar challenges or who can simply understand what you’re coping with. Your local hospital or your loved one’s physician can usually point you in the direction of support groups designed for caregivers in your area. In addition, MeetUp.com often lists local support groups, or you can create a group if it doesn’t already exist in your area. If getting out to meet in person is difficult, various online support groups are available, such as The Caregiver Space, the Smart Patients Caregiving Community and Caregiving.com.
2) Respite Care
Many insurance plans offer respite care benefits. Medicare and Medicaid will provide them under specific circumstances as well. Respite care is a special type of temporary care provided for people with disabilities or life-threatening illnesses. Although the duration of relief care varies, it often gives caregivers a few days or couple of weeks each year to rest, travel, or see to their own personal needs. If your insurance does not cover respite care, see Julia Quinn-Szcesuil’s Care.com article “How Do I Pay for Respite Care?”
3) In-Home Healthcare
Like respite care, in-home healthcare is often a covered benefit of insurance plans, including Medicare and Medicaid plans. It can help bridge the gap between enabling someone to stay at home and recovering in a skilled rehabilitation center or staying in a nursing home. While it’s not ideal for someone who needs around-the-clock care, it can help caregivers make ends meet, as the healthcare specialist can assist with things like bathing and dressing wounds during a visit. Philip Moeller walks a caregiver through the process of setting up in-home healthcare through Medicare on PBS News Hour.
4) Local Area Agency on Aging
Your local Area Agency on Aging can provide a wealth of information and connect you with all sorts of resources, ranging from assistance understanding benefits that are available to finding care providers and services in your area. To find your local resource, visit the National Association of Area Agencies on Aging website and enter your location.
5) FMLA
Most people have to work a paid job in addition to caregiving, and that presents unique challenges as well. Between needing time off for surgeries and doctor appointments to managing affairs and providing physical care, flexibility from employers is often needed. The Family Medical Leave Act (FMLA) provides a pathway for people caring for others to take time off when they need it, without worry about losing their job.
6) Benefits Checkup
With so much going on and so many things to track, it’s easy to overlook a benefit or service you may be entitled to that can ease some of your burden. The Benefits Checkup provided by the National Council on Aging lets you enter your location to see all programs in your area you or your loved one may qualify for.
7) RefillWise
Oftentimes, insurance plans and medical programs leave a gap, and not everyone is fortunate enough to have coverage either. Expenses for things like medical equipment and prescriptions add up fast. If you’re a caregiver acting as head-of-household, you may also be struggling with the cost of pet medications, and general household expenses too. RefillWise can help with all these things. Our free pharmacy discount card works on all prescription medications, as well as prescription medical equipment, and can be used at most popular pharmacies — saving you money whether you need to make purchases for yourself, your family, the person you’re caring for, and even your pets. Best of all, our rewards program offers you cash back for using our card, which you can use on all your other needs, from groceries to hygiene supplies, clothing, or little treats for yourself. To get started, text JOIN to 22822 or sign up on our site now.
Although the FDA cautions against the practice, and 62% of the population believes it’s less safe than purchasing from a brick-and-mortar pharmacy, buying prescriptions drugs online is like a siren call to millions every year according to Pew Research. Some say they do it to get affordable prescriptions, while others cite things like convenience and privacy, but what they may not know is that they could pay the ultimate price for those would-be benefits.
1) Some Drugs are Formulated with Toxic Ingredients
The greatest danger in purchasing drugs online is that there is no guarantee the pharmacy is based in the United States or that any controls are in place to test the validity of the drug. According to Consumer Reports, “dangerous contaminants, including toxic yellow highway paint, heavy metals, and rat poison” are included in some mixes.
2) Dosing is Not Always Accurate
In pharmacies with little or no oversight, it’s not uncommon to find drugs that contain varying amounts of the active ingredient. At best, this could render the medications ineffective. At worst, it leads to deadly overdoses.
3) An Online Pharmacy May Prevent You from Getting the Help You Need
“Using unproven treatments can delay getting a potentially life-saving diagnosis and medication that actually works,” cautions Gary Coody, R.Ph., the FDA’s national health fraud coordinator. He was speaking of fraudulent medications, especially those that make bogus claims about what the substance can do. This is common with drugs sold to enhance sexual performance or aid in weight loss, but it’s also seen with substances marketed as cures for things like Alzheimer’s disease, diabetes, and other serious conditions. Always beware of drugs that seem too good to be true, tout themselves as a miracle cure, claim to be an ancient remedy, or promise instant results.

4) You Can’t Tell How a Medication was Handled
Many medications require a specific environment to maintain their potency. Oftentimes, this means that they must be kept away from heat and sunlight, or even refrigerated. When medications are shipped from unknown pharmacies, it’s difficult to know if they were handled properly, both by the company and by the shipper.
5) The Medications You’re Buying May Be Illegal
If you’re obtaining prescription drugs and you do not have a valid prescription for them, you’re breaking US law by bringing them into the country. It’s also illegal to bring medications in that aren’t approved by the FDA. Either situation could land you in hot water with the federal government.
6) 96% of Online Pharmacies are Considered “Rogue”
The National Association of Boards of Pharmacy (NABP) makes a point of researching as many online pharmacies as it can to see if they’re legit. At last count, the non-profit had checked nearly 11,500 outlets and discovered that roughly 96% are not compliant with US pharmacy laws. In other words, if you buy online, there’s only a 4% chance you’re buying from a legal pharmacy.
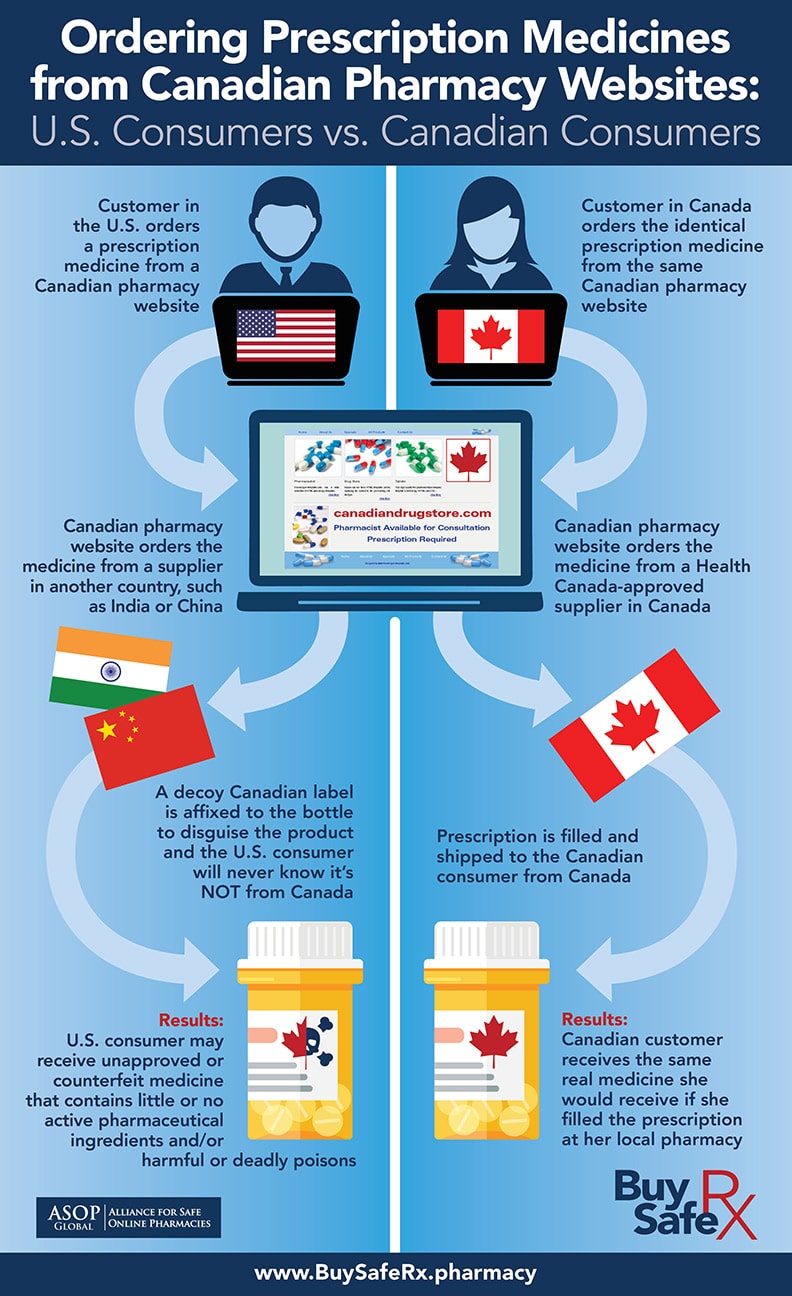
The Association for Safe Online Pharmacies (ASOP) in this infographic describes how international pharmacies, like those in Canada, take advantage of the lack of regulations to secretly send American consumers potentially unsafe medicines from India or China.
Get Affordable Prescriptions with Help from RefillWise
RefillWise only partners with reputable brick-and-mortar pharmacies, so you can be sure that you’re always getting the medications you need in a safe and affordable way. Our cardholders save an average of 40% on prescriptions, medical equipment, and pet medicines. If you’d like to begin saving as well, text JOIN to 22822 or sign up on our site today.





